Monoclonal antibodies are a pool of antibodies specific for the same epitope as they are originally produced by a single B-lymphocyte cell. Like for polyclonal antibodies a host animal has to be immunized first to receive the antibody producing cell (see Figure 1 step 1 and 2). This cell is then fused with a tumor cell of the same host (see Figure 1 step 4).
In 1975 G. Köhler and C. Milstein published in Nature the introduction of a hybridoma technique to produce monoclonal antibodies. This technique has become a pillar in modern biological science, the diagnosis of diseases and the actual therapy of various illnesses. The authors fused a mouse myeloma with a mouse spleen cell (both of BALB/c origin) to obtain a number of cell lines secreting antibodies against sheep red blood cells (see Figure 1 step 4 and 5). The result of this fusion was a hybrid cell line, called a hybridoma, that stably expressed monoclonal antibodies. The hybridoma cells could then be injected into BLAB/c mice to produce antigen-specific serum or hybridized to antibody-producing cells from different origins to induce the in vitro production of antibodies. Georges Köhler, César Milstein, and Niels Kaj Jerne shared the Nobel Prize in Physiology or Medicine in 1984 for the discovery.
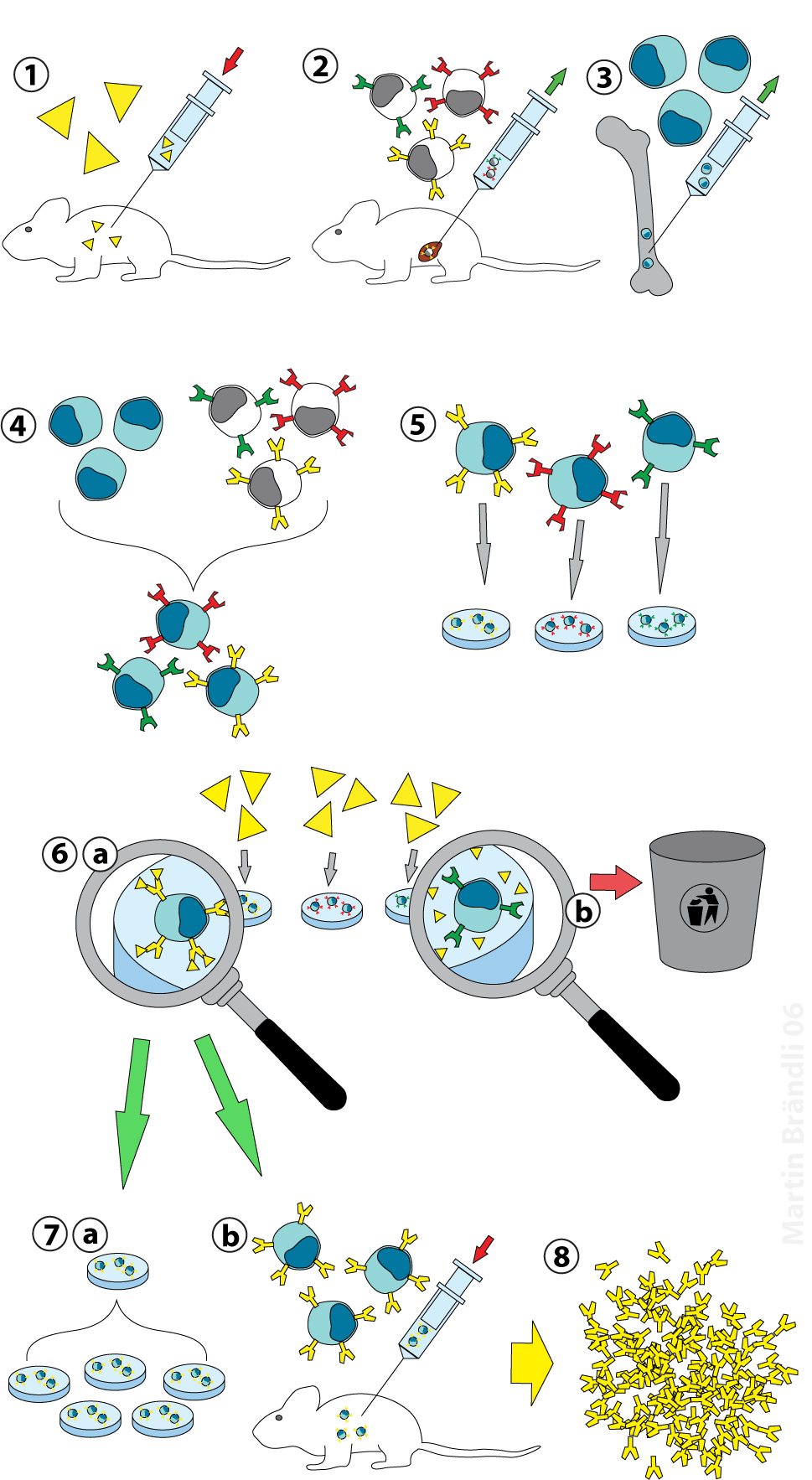
Abbildung 1: Principle of the hybridoma-technique By Martin Brändli (Own work) [CC-BY-SA-2.5 (http://creativecommons.org/licenses/by-sa/2.5)], via Wikimedia Commons
Hybridoma cells synthesize the specific monoclonal antibody originally produced by the B-lymphocyte cell. The original B-lymphocyte cell will produce the monoclonal antibody depending on the antigen that was injected into the host prior to the harvesting of the B-lymphocyte cells. If e.g. the host is exposed to a replicating virus it will develop B-lymphocytes that produce specific viral antibodies. Fusion with a tumor cell to make the hybridoma results in the production of monoclonal antibodies against the specific virus.
Custom Antibody Services
Custom Antibody Services
Benefit from combined expertise of antibodies-online and our Partner Rockland Immunochemicals, Inc. Collaborative, experienced, and conducted completely in our own facilities, our custom antibody production services can drive your project from the design and synthesis of your antigen through to production and characterization of your antibody.
Benefit from combined expertise of antibodies-online and our Partner Rockland Immunochemicals, Inc. Collaborative, experienced, and conducted completely in our own facilities, our custom antibody production services can drive your project from the design and synthesis of your antigen through to production and characterization of your antibody.
Hybridoma cells are then selected by epitope affinity and after another round in a selective culture in hypoxanthine-aminopterin-thymidine medium (HAT medium). Aminopterin blocks DNA de novo synthesis which is required for cell division, while hypoxanthine and thymidine provide cells with the raw material to bypass the blockage if the cell harbors the essential functional enzymes. Unfused myeloma cells do not produce the right enzymes while the unfused spleen cells cannot grow indefinitely. Thus, only hybridoma cells will grow indefinitely in the media.
As described above there are two methods for growing hybridoma cells (here described for the common host mouse): 1) injecting them into the peritoneal cavity of a mouse (see Figure 1 step 7b) or 2) using in vitro cell-culture techniques (see Figure 1 step 7a). The cell-culture technique needs some expertise, requires special media, and can be expensive and time-consuming. Although the cell culture method is widely preferred, a number of monoclonal antibodies will still be produced in vivo in mice. When injected into a mouse, the hybridoma cells multiply and produce fluid (ascites) in its abdomen; this fluid contains a high concentration of antibody (often a 10 fold higher concentration than obtained in cell culture supernatants).2 The Institutional Animal Care And Use Committee (IACUC) created a guideline, under which conditions the in vivo production of monoclonal antibodies is acceptable.
By now monoclonal antibodies are widely used for research, diagnostics and therapies. A drawback of the commonly used mouse antibodies for therapeutic applications is the human immune response due to the minor structural differences between human and murine antibodies. In 1988, Greg Winter and his team pioneered the techniques to humanize monoclonal antibodies, thus minimizing the reactions that many monoclonal antibodies caused in patients. In one approach, mouse DNA encoding the binding portion of a monoclonal antibody was recombined with human antibody-producing DNA in living cells. That yielded partially mouse, partially human monoclonal antibodies when expressed in cell culture. These products are called chimeric antibodies. By now chimeric antibodies can be produced in various host species, not only mouse and human.
Many protein targets related to signal transduction and disease are highly conserved between mice, humans and rats. They can therefore be recognized as self-antigens if the host is a rat or mouse and are consequently less immunogenic. Until now a number of hybridoma cells from different host animals have been introduced to overcome the limitation of antigen recognition in mouse. On the other hand plant antigens are sometimes less immunogenic in herbivores and omnivores or carnivores therefore better catered to produce such antigens.
Info: Antibodies-online.com offers more than 100.000 monoclonal antibodies.
Featured Monoclonal Antibodies
- (122)
- (8)
- (4)
- (4)
- (2)
- (8)
- (15)
- (1)
- (126)
- (12)
- (3)
- (4)
- (1)
- (6)
- (2)
- (10)
- (1)
- (7)
- (2)
- (7)
- (1)
- (60)
- (5)
References:
: "Continuous cultures of fused cells secreting antibody of predefined specificity. 1975." in: Journal of immunology (Baltimore, Md. : 1950), Vol. 174, Issue 5, pp. 2453-5, (2005) (PubMed).: "Reshaping human antibodies for therapy." in: Nature, Vol. 332, Issue 6162, pp. 323-7, (1988) (PubMed).
: "Therapeutic antibody expression technology." in: Current opinion in biotechnology, Vol. 12, Issue 2, pp. 188-94, (2001) (PubMed).
Monoclonal Antibody Production; National Research Council (US) Committee on Methods of Producing Monoclonal Antibodies. Washington (DC): National Academies Press (US); 1999. ISBN-10: 0-309-07511-4 ISBN-13: 978-0-309-07511-4 ISBN-10: 0-309-51904-7, Available from: http://www.ncbi.nlm.nih.gov/books/NBK100200/
http://iacuc.utk.edu/policies-and-procedures/guidelines-for-in-vivo-monoclonal-antibody-production/

Goal-oriented, time line driven scientist, proficiently trained in different academic institutions in Germany, France and the USA. Experienced in the life sciences e-commerce environment with a focus on product development and customer relation management.
Go to author page



